At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What Happens to Donated Blood?
When a person donates blood, it's just the beginning of a much longer process to get the blood to a person in need. Donated blood must undergo several steps. First, some of the blood is tested, and the rest of the donation is processed. Then the blood is stored before it finally is used to help people with a medical need for blood or blood components.
At the time of donation, donors must provide information about their health and blood type and whether they have certain diseases. In order to keep the blood supply safe, the donated blood is thoroughly tested for a variety of diseases and to confirm the type. This is done in case donors are mistaken about their blood type or in case they have contracted a disease that they aren't aware of yet. Donated blood is tested for the Rheses (Rh) factor; for common blood types A, B, AB and O; and for unusual antibodies and blood types. If any of the test results are positive for a disease, the donor is notified, and the donation is not used.

Some of the infectious diseases, or disease causing agents, the donated blood is tested for include type 1 and type 2 human immunodeficiency virus (HIV), the virus that causes acquired immunodeficiency syndrome (AIDS), and hepatitis B and C. Other diseases tested for are West Nile virus, syphilis, Chagas disease, and human T-lymphotropic virus. The tests performed look for antibodies that an exposed person's system will create. In some cases, they also look for nucleic acids created by the virus itself. These tests are necessary because a person can be exposed to these agents but not show symptoms, and these agents can sicken a person when they are received through blood transfusion.

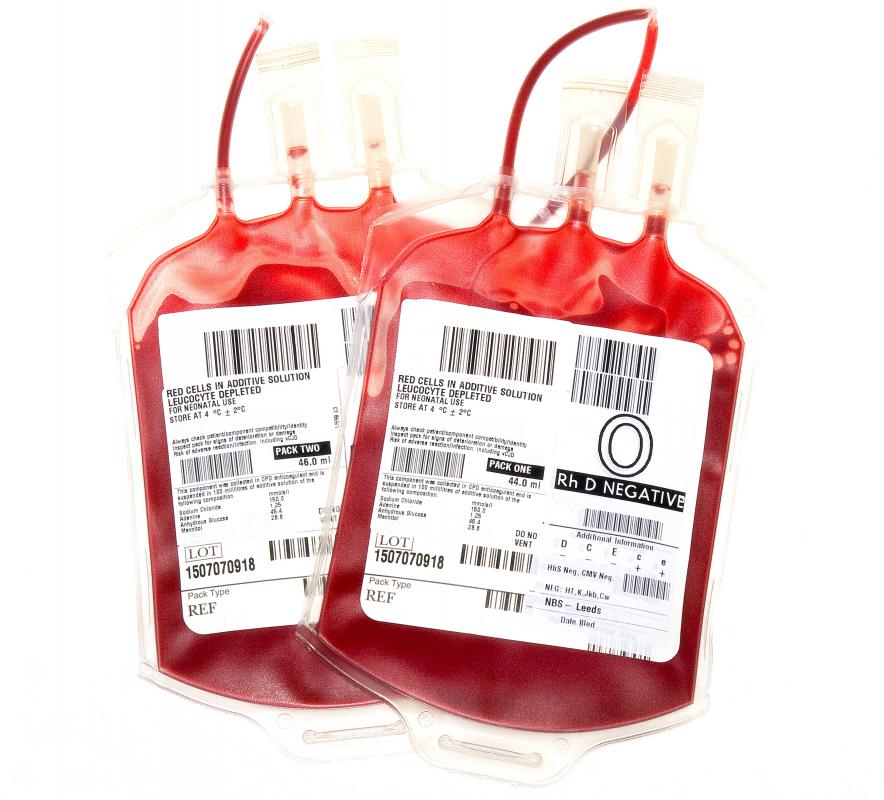
During testing, the rest of the donated blood usually goes through processing, where it is prepared for use or can be stored as whole blood. During processing, the donated blood is separated into parts or components, such as red cells, platelets and plasma, by spinning it in a centrifuge. The plasma also can be processed further into a substance called cryoprecipitate. Components also undergo a process called leukoreduction, which is the removal of white blood cells so that they don't interfere with the patient's immune system. The separated components then can be used to treat multiple patients with different conditions, so one pint of blood can help more than one patient.

Next, the donated blood goes into storage until it is needed. Storage methods and times vary depending on the blood component. Platelets need to be stored at room temperature and kept in constant motion in an agitator, and they last for only five days. Whole blood needs to be refrigerated and can be stored safely for as long as 35 days, and red blood cells can be refrigerated for as long as 42 days. Plasma and cryoprecipitate have the longest storage time — as long as one year — and are frozen.

Finally, when it is needed, the donated blood is distributed to hospitals to be used in treating a variety of conditions. Whole blood often is needed for surgery patients and trauma victims. Red blood cells are useful in the treatment of both sickle cell anemia and standard anemia as well as for any other significant blood loss. Platelets are used to treat certain cancers, such as leukemia; plasma is used for clotting disorders and burn patients; and cryoprecipitate is very useful in the treatment of hemophilia. Many blood banks are able to ship whole blood and blood components to hospitals every day, at any time.
AS FEATURED ON:
AS FEATURED ON:
















Discussion Comments
I would like to be able to donate blood, but I'm on a good many medications and they won't let me.
My mom worked in a hospital in the 50s and 60s, and said she remembers a couple of times when they had a critical case, that the state highway patrol would set up a blood relay, in case no blood of the required type was available in their hospital. She said it wasn't unusual for a rare type, like AB negative to be relayed from 100 miles away. I don't think that happens too often now, thank goodness, but it wasn't terribly unusual then.
Post your comments