At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is Trigger Thumb?
Trigger thumb is a condition in which the thumb is locked, usually in a bent position, due to a localized swelling of flexor pollicis longus tendon that limits its excursion within the flexor tendon sheath. It is mainly characterized by locking or painful triggering of the thumb and can cause significant impairment of hand function, especially for those individuals whose hobbies or work need repetitive gripping. Its cause is usually unknown, but may be associated with certain metabolic and inflammatory diseases. Risk factors include repetitious gripping and certain diseases, and women are more affected. Treatment of this condition depends on the degree of its severity and duration.
The position of the locking of the thumb depends on the location of the swelling on the tendon. If it is proximal to the flexor tendon sheath, the thumb is locked in a bent position. In case it is within the flexor tendon sheath, the thumb is locked in a straight position. Aside from painful triggering and locking, other signs and symptoms of trigger thumb include morning stiffness of the thumb, clicking or popping as the thumb is moved, tenderness or a nodule that moves with bending or straightening of the thumb, and active snapping.
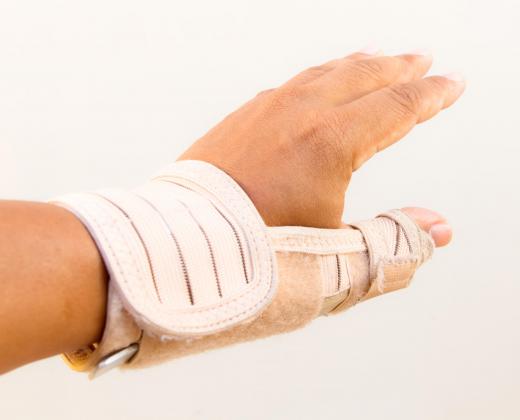
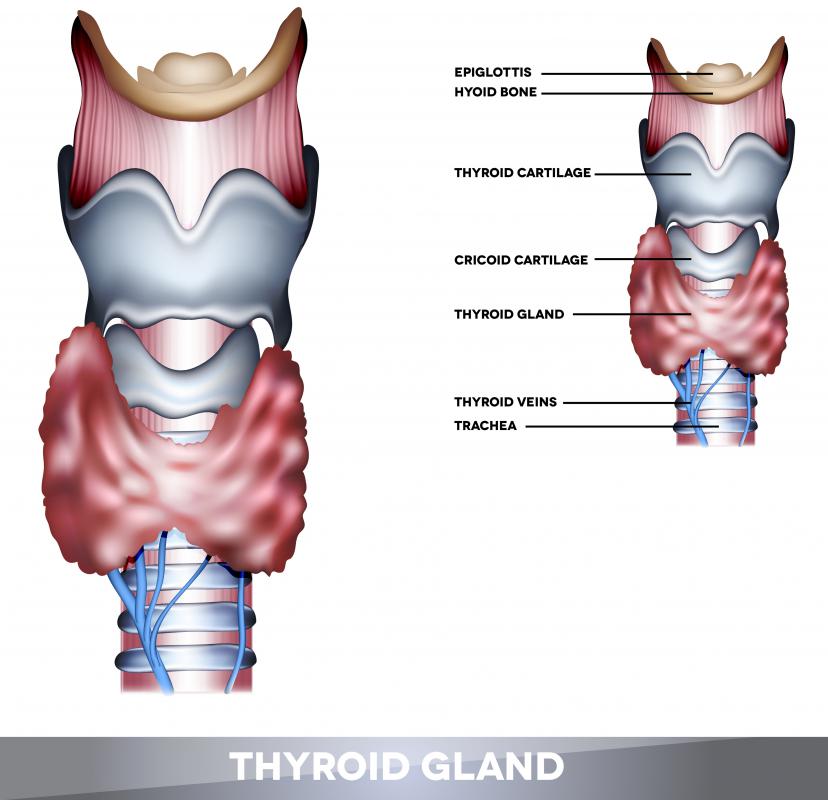
Trigger thumb usually affects the dominant hand, but other fingers may also be involved. Individuals whose hobbies or work need repetitive gripping are at high risk for this condition. Certain metabolic and inflammatory conditions, such as diabetes, hypothyroidism, rheumatoid arthritis, amyloidosis, gout, or chronic infection, cause inflammation of the tenosynovium, leading to a narrowed and constricted space within the tendon sheath, thereby limiting the gliding movement of the tendon. The tenosynovium lines the tendon sheath and secretes a lubricating fluid for the smooth gliding movement of the tendon. Women are four times more likely to develop a trigger thumb.

Diagnosis of trigger thumb is usually based on history and physical examination. Laboratory tests are generally not ordered for trigger thumb with unknown cause. Imaging modalities and laboratory tests are not necessary, but they help confirm or exclude the suspicion of associated metabolic or inflammatory conditions.
For mild cases of trigger thumb, treatment is usually non-pharmacological. This includes resting the affected hand for 4 to 6 weeks, changing and avoiding work or hobbies that need repetitive gripping or grasping actions for at least 3 to 4 weeks, splinting for up to 6 weeks, performing gentle finger exercises, soaking in warm water especially in the morning, and massaging. For serious cases of trigger thumb, treatment includes pharmacological and/or surgical approaches. Pharmacological approaches include the use of nonsteroidal anti-inflammatory drugs or steroids to relieve symptoms, and surgical approach includes the surgical release of the affected tendon.
AS FEATURED ON:
AS FEATURED ON:
















Discuss this Article
Post your comments